The Low FODMAP Diet: A How To Guide!

Gut health!
It’s the new kid on the block, and everyone is flocking to monetising the movement with self-proclaimed titles like ‘gut health guru’. It’s become the latest marketing strategy of the decade, and people LOVE it. Amongst some of the wild claims circling in this movement *insert leaky gut diagnosis* is the idea that everyone should avoid fodmaps, otherwise known as fermentable oligosaccharides, disaccharides, monosaccharides and polyols (yep, let’s stick with FODMAPS).
This blog intends to highlight the evidence around fodmaps:
- What are they?
- Why do they matter?
- And should we be including these types of foods in our diets?
So let’s jump into it!
Before we jump into the main topic of this blog, I want to highlight one essential thing:
- Most bloating is a very normal process that occurs when we ingest and digest food. It is entirely normal to have some bloating after eating a large meal, and your abdomen will look more prominent at the end of the day than it did in the morning.
It’s essential to bring light to this because some health gurus will have you believe that any bloating requires investigating. Bloating becomes a problem when accompanied by pain, decreased quality of life, chronic constipation or diarrhoea. A low FODMAP diet should be considered if your symptoms are so bad that they affect your quality of life, not to cure typical bloating.
Ok, now that we have got that out of the way, let’s jump into it.
What are FODMAPS?
Fodmaps are a group of short-chain carbohydrates found in many common foods. These carbohydrates are a necessary food for our gut microbes, as they’re fermented by the bacteria in our large bowel. Our gut requires a large diversity of gut microflora to thrive and remain healthy. So fermentation of bacteria in our gut (while it sounds funky) is great for gut health!
FODMAPS are safe for most people to eat, but they can cause digestive problems for those with irritable bowel syndrome (IBS). Irritable bowel syndrome (IBS) is a common disorder that affects the large intestine. Symptoms include abdominal pain, cramping, bloating, gas, diarrhoea, and constipation. When these carbohydrates are not adequately digested, they can pull water into the intestine, leading to gas, bloating, and abdominal pain. Common foods that contain FODMAPs include garlic, onions, wheat, and dairy products. IBS can be debilitating, making it difficult to work, socialise, and even travel. There is no cure for IBS, but there are treatments that can help to manage the symptoms. The low FODMAP diet is designed to help people suffering from Irritable bowel syndrome (IBS) by limiting the number of fermentable sugars in their diets. This can reduce pain and other symptoms that may come along with it, such as bloating or diarrhoea!
Examples of HIGH FODMAP Foods
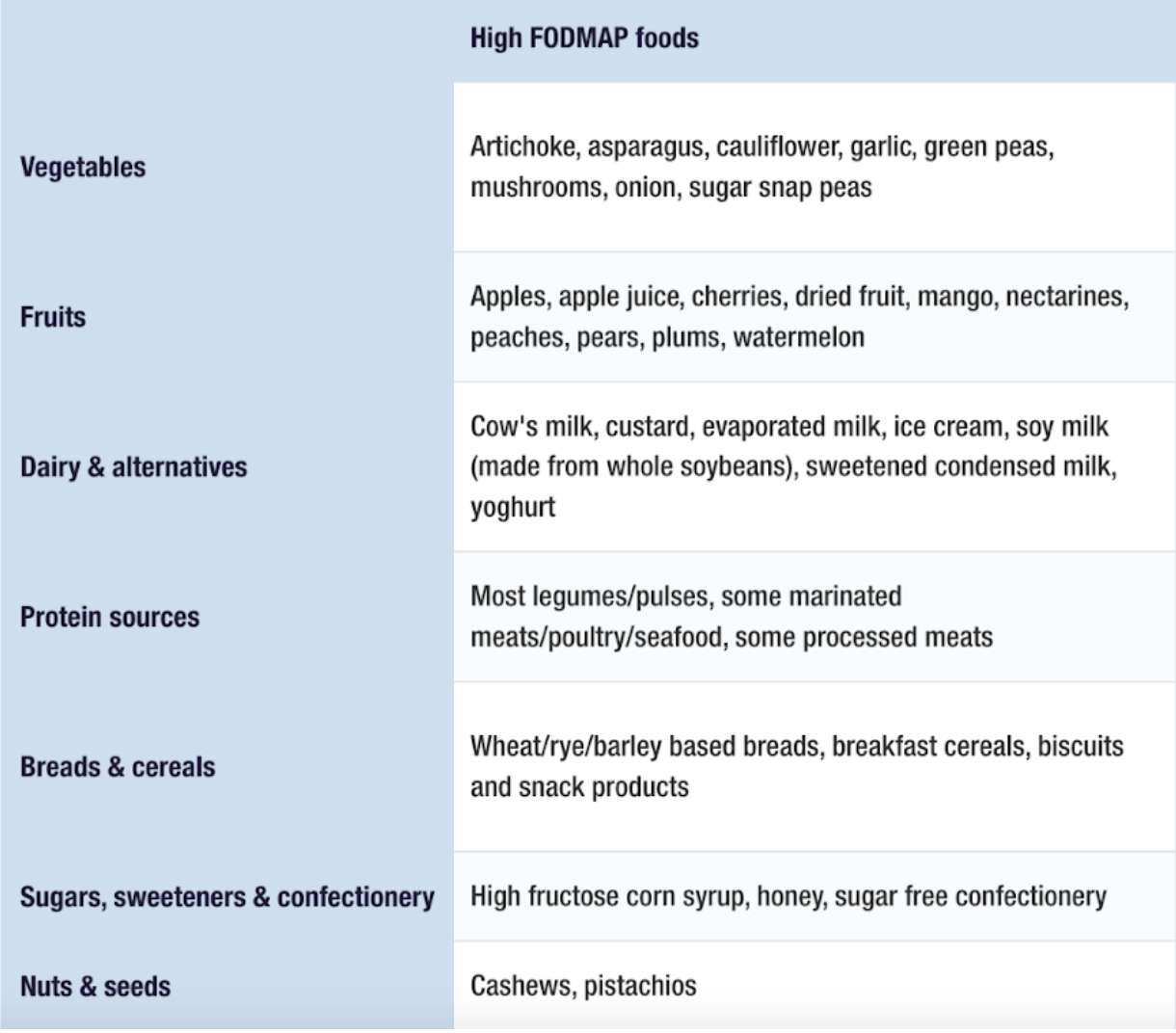
Examples of LOW FODMAP Foods
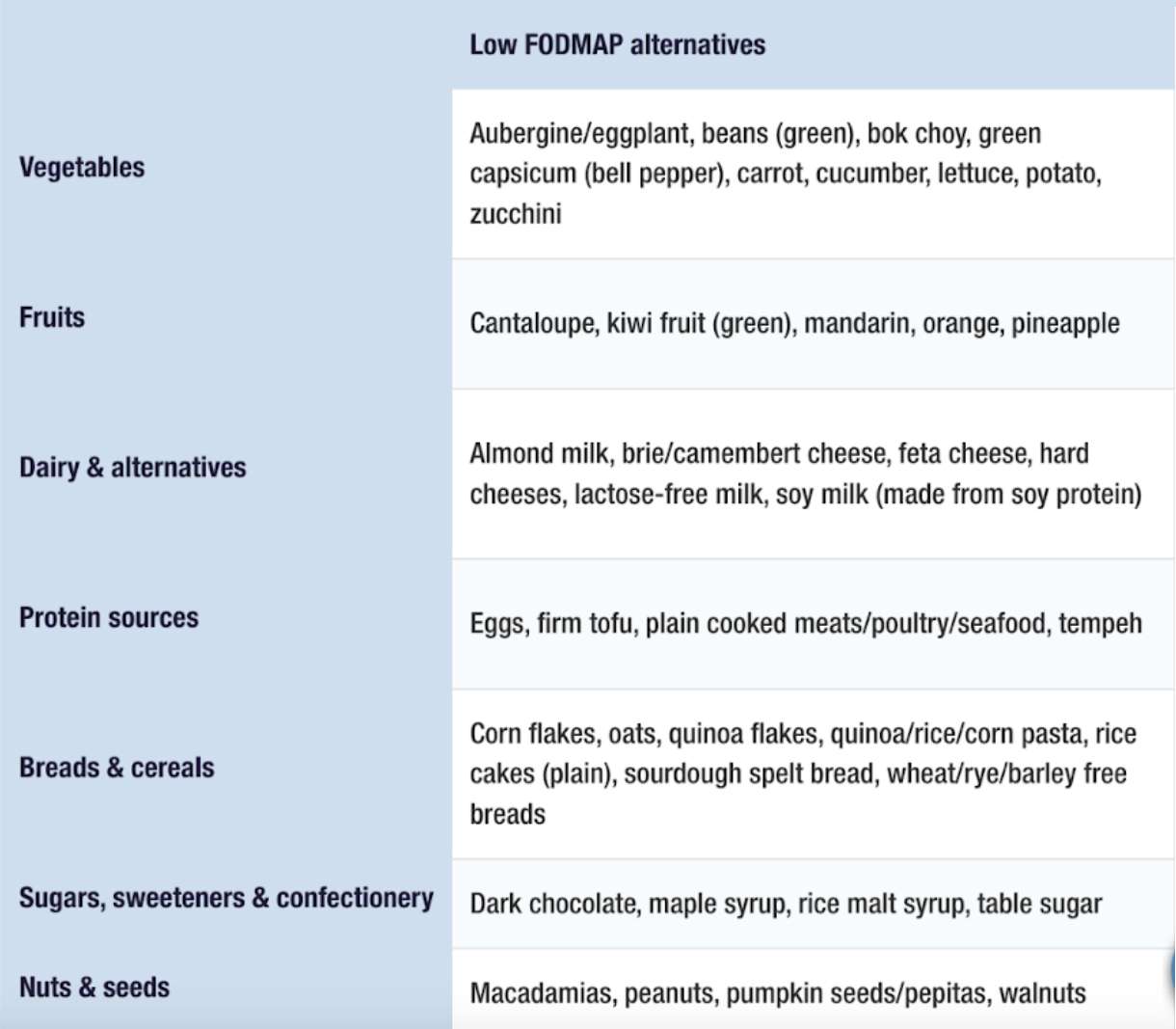

Credit: Monash University
How does the low FODMAP diet work?
Let’s start by outlining that the low FODMAP diet isn’t actually a diet at all! It’s more of a protocol. This means that you should only follow a low FODMAP diet for a short period of time. This is where advice from coaches who need to be better educated in this area goes wrong.
The low FODMAP diet phase one:
The first phase of a low FODMAP diet starts by eliminating all high FODMAP foods for a period of 2-4 weeks (yes, 2-4 weeks).
Phase two:
The second stage involves reintroducing these foods slowly. This allows you to identify which FODMAPS you are sensitive to. Each person responds differently to FODMAPS, and the amounts that each person can tolerate will also differ. Therefore, it’s essential to find the dosage that’s appropriate for you. In addition, it’s essential to pay attention to the symptom you experience and how long it lasts. For some, a symptom might present as abdominal cramping and bloating. For others, it results in loose stools, which is never fun for anyone in social situations. It helps to keep a symptom, dosage and food diary in the reintroduction phase. This will give you a road map into what FODMAPS you should eliminate or reduce to manage IBS symptoms.
Phase three:
This step requires you to personalise the FODMAPS that are relevant to you. It’s unlikely that someone with IBS symptoms cannot tolerate every FODMAP. You will need to consider if you will consume, reduce or eliminate the particular FODMAP based on phase two.
What are the long-term consequences of following a low FODMAP diet?
Many FODMAP foods are super beneficial for our gut bacteria. While there is so much we don’t know about gut health, we do know that a diverse range of plant foods is imperative for a thriving gut microbiome. Suppose we remove these foods over an extended period. In that case, we are removing the diversity of bacteria housed in our gut. This comes with its own health implications, so it is important not to exclude foods just for the sake of it. Consuming a low FODMAP diet also creates stringent and restrictive rules around food, which can increase the risk of developing eating disorders. There are also several other reasons for GI discomfort such as coeliac disease and Crohn’s disease, so you should take steps to have other conditions ruled out before assuming IBS is the culprit. These are just a few reasons that a low FODMAP diet should be done under the guidance of a dietician and a gastroenterologist.
Yours in Health,
Sheridan Skye.
Head of Nutrition at CMC and Registered Nurse.







